
What Blood Type Are You?
If you ever need a transfusion, knowing your specific Blood Type could be a matter of life and death. But many people believe that knowing which Blood Type you are can determine your personality and seriously effect the way your body reacts to disease and processes food.
In this article, I'll explore the history and significance of different blood types, their possible evolutionary origins and purpose, as well as their significance when it comes to diet and disease. Our interest is mainly in exploring the social and medical considerations of your blood type and how you can use this information to improve your health.
Asian cultures, most notably Japanese, put much weight on the acquisition of personality traits through an individual's Blood Type. Type A is considered petty, selfish, bearing grudges and suppressing anger yet romantic; Type B are considered carefree but prone to random anger and nervousness; Type O are athletic, inquisitive, goal oriented and like to talk to vent their feelings.
This humorous video [below] describes the belief, in Japan, that blood types have distinct personality traits.
In some reports on-line I've read where candidates who otherwise were qualified for a particular job were refused because the employer was looking for a "different blood type".
Because certain blood types are concentrated in different geographic regions of the world, these personality traits could more likely represent varied cultures and adaptations to different environments. This is an area of research which has not been seriously explored.
|
Where is your blood type from?
We have learned a good deal about how common each of the ABO blood types is around the world. The patterns can thus be traced to specific regions, migrations and intermingling of various civilizations in human history. This can be seen with the global frequency patterns of the type B blood allele (shown in the map below). Note that it is highest in Central Asia and lowest among the indigenous peoples of the Americas and Australia. However, there are relatively high frequency pockets in Africa as well. Overall in the world, B is the rarest ABO blood allele. Only 16% of humanity have it.
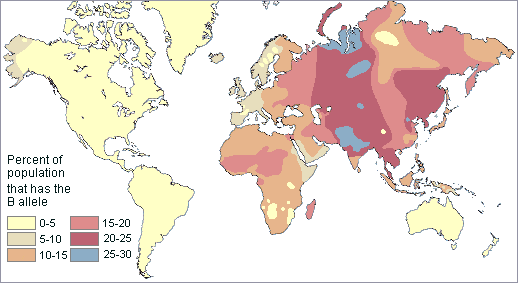
Distribution of the B type blood allele in native populations of the world The A blood allele is somewhat more common around the world than B. About 21% of all people share the A allele. The highest frequencies of A are found in small, unrelated populations, especially the Blackfoot Indians of Montana (30-35%), the Australian Aborigines (many groups are 40-53%), and the Lapps, or Saami people, of Northern Scandinavia (50-90%). The A allele apparently was absent among Central and South American Indians.
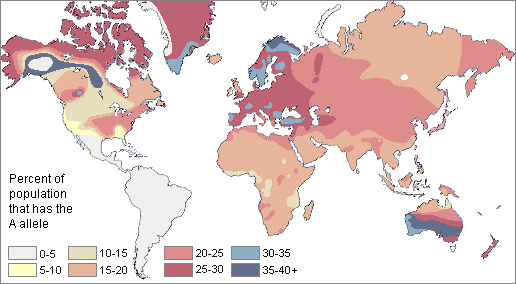 Distribution of the A type blood allele in native populations of the world The O blood type (usually resulting from the absence of both A and B alleles) is very common around the world. About 63% of humans share it. Type O is particularly high in frequency among the indigenous populations of Central and South America, where it approaches 100%. It also is relatively high among Australian Aborigines and in Western Europe (especially in populations with Celtic ancestors). The lowest frequency of O is found in Eastern Europe and Central Asia, where B is common. As we'll see later, type O is considered the original blood flowing in both Neandertal and Cro-Magnon primates.
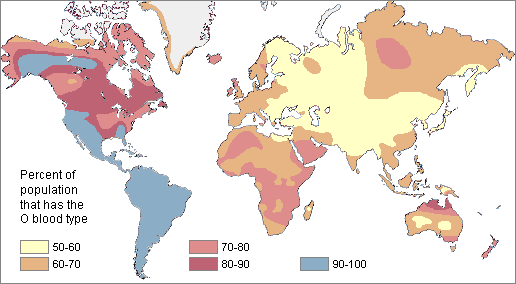 Distribution of the O type blood allele in native populations of the world
[source Wikipedia]
|
A great deal of peer reviewed literature exists on the correlation between blood types and specific diseases. Knowing your blood type and the type of illnesses associated with it could potentially be beneficial when considering the last claim: that certain foods are either good or bad. We'll come back to this diet theory, but first lets look at a brief history of blood types and examine the reports of various illnesses.
The History of Blood
Early medicine realized the life-giving properties of the red liquid that was inside our flesh. Before the concept of circulation was understood, the maladies of blood related illness were attributed to whether there was too little or too much blood in the patient. Applying leaches to the skin was thought to be a remedy for excess blood, but a treatment for too little blood remained unsolved.
The earliest recorded attempt to increase the blood volume in an ill patient happened in the same year that Columbus discovered America, 1492. Historian and writer, Stefano Infessura, describes how the ailing Pope Innocent VIII was diagnosed with too little blood when he became comatose. Desperate to save his life, the fresh blood of three preteen boys was collected by bleeding them. Because the concept of arteries, veins and circulation was unknown, the donated blood was administered orally, through a tube down the Pope's throat. The experiment was a total failure and somehow all four people died.
Less than two hundred years passed before the second series of documented transfusions were performed. In 1667 the blood of sheep and cattle was transfused into a variety of patients by the French physician, Jean-Baptiste Denys. A little animal blood seemed to do no harm, but repeated and larger doses were deadly. Many people died and the procedure was banned in 1670.

If we leave the "human" element out of it, the first successful transfusion was actually made in 1665 between two dogs. Christian Zagado had perfected a closed, airtight system with tubes that eliminated clotting and embolisms. A physician named Lower transfused the dogs in the presence of the French Royal Society using Zagado's system.
"Many of his colleagues were present. towards the end of February 1665 he selected one dog of medium size, opened its jugular vein, and drew off blood, until... its strength was nearly gone . Then, to make up for the great loss of this dog by the blood of a second, I introduced blood from the cervical artery of a fairly large mastiff, which had been fastened alongside the first, until this latter animal showed... it was overfilled... by the inflowing blood... sewed up the jugular veins... the animal recovered with no sign of discomfort or of displeasure."
Remember Denys, whose animal to human transfusions were so deadly? Denys redeemed himself by taking credit for the first successful human to human exchanges in 1667, but both he and Lower continued to dabble in interspecies experiments. Clearly, blood transfusions were not safe and most did not benefit the patient.
In 1901 the mortality rate from blood transfusions dropped with the discovery by Austrian Karl Landsteiner that blood from two different individuals can sometimes form clumps or agglutination, inducing a toxic reaction, clots and death. This led to the classification of four distinct types called type A, B, both A&B, or neither (type O), depending on the observed antibodies. Matching blood types finally made transfusions safe and earned Landsteiner the 1930 Nobel Prize in Physiology or Medicine.
Though it was not always terminal, reactions to some transfusions were still occurring despite matching the A-B-AB-O blood type. In 1940, Karl Landsteiner zeroed in on the so-called Rhesus factor (Rh) which, if present or not, must also be considered for a safe transfusion match.
This resulted in eight possible blood types: A-, A+, B-, B+, AB-, AB+, O-, O+.
TYPE
|
CAN RECEIVE FROM |
CAN DONATE TO |
Comments: |
A-
|
A-, O- |
A-, A+, AB- |
|
A+
|
A+, A-, O-, O+ |
A+, AB+ |
|
B-
|
B-, O- |
B-, B+, AB- |
Rarest type
|
B+
|
B-, B+, O-, O+ |
B+, AB+ |
Rare 16%
|
AB-
|
AB-, B-, A-, O- |
AB- |
|
AB+
|
AB+, AB-, B+, B-, A+, A-, O+, O- |
AB+ |
Universal recipient
|
O-
|
O- |
A+, A-, B+, B-, AB+ AB-, O+, O- |
Universal donar |
O+
|
O-, O+ |
A+, B+, AB+, O+ |
Most common type
|

Are You At Risk?